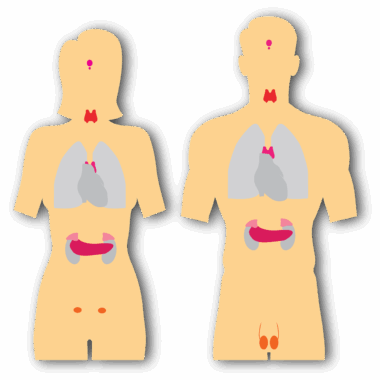
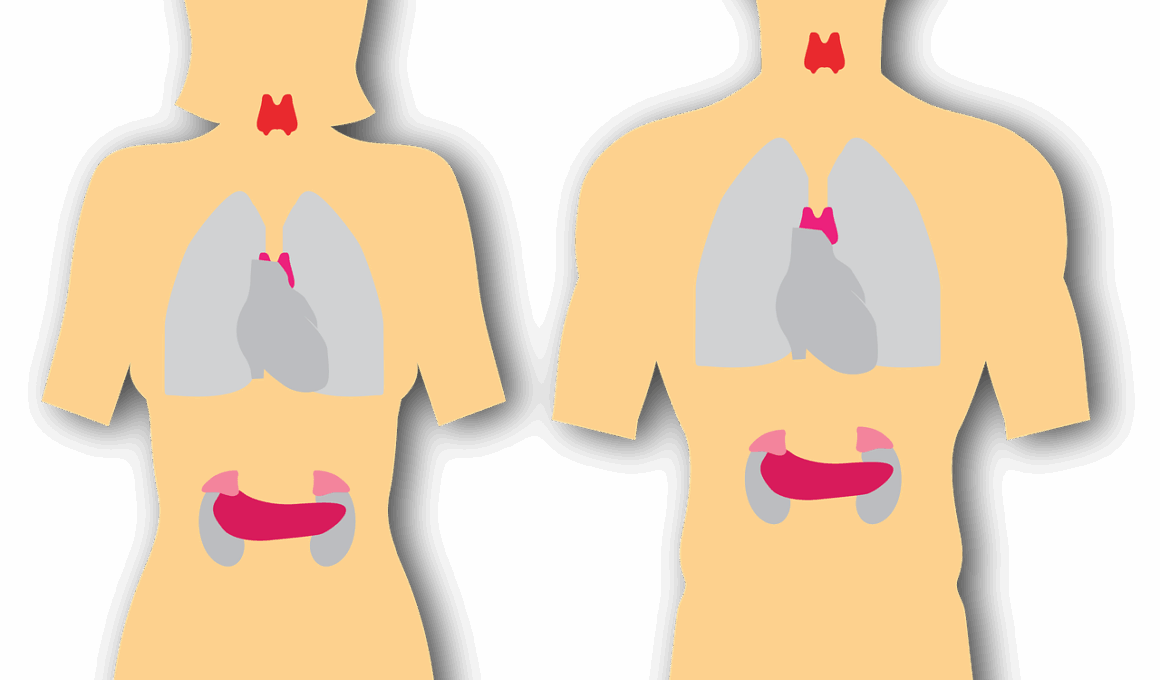Endocrine Functions of the Gonads: Testes and Ovaries
The endocrine system plays a crucial role in regulating various physiological processes through hormonal secretion. In both males and females, the gonads, which include the testes in males and ovaries in females, are central to this function. The testes primarily produce testosterone, influencing the development of male secondary sexual characteristics and regulating sperm production. This hormone plays a vital role in libido and reproductive functions. In contrast, ovaries are responsible for the production of estrogen and progesterone, which regulate the menstrual cycle and pregnancy. These hormones also influence secondary sexual characteristics in females, such as breast development and fat distribution. The functions of these hormones are intricately connected to overall health and reproductive well-being. Hormonal imbalances can lead to various health issues, including infertility and developmental disorders. Thus, understanding the endocrine functions of the gonads is essential for addressing related medical conditions. The interplay between these hormones illustrates the complexity of the endocrine system, highlighting the importance of both testes and ovaries in human physiology. Further studies in this area can lead to advancements in reproductive health and endocrinology.
Hormonal Regulation in Males
The testes are primarily involved in the production and regulation of testosterone, which is essential for male reproductive health. Testosterone influences the development of male genitalia during embryogenesis and is crucial for spermatogenesis after puberty. In the hypothalamus, the release of gonadotropin-releasing hormone (GnRH) stimulates the pituitary gland to produce luteinizing hormone (LH) and follicle-stimulating hormone (FSH). LH directly stimulates the Leydig cells in the testes to produce testosterone, while FSH acts on Sertoli cells to facilitate sperm maturation. The levels of testosterone in the bloodstream are carefully balanced through a feedback loop involving the hypothalamus and pituitary gland. This regulatory mechanism ensures sufficient hormone levels, which are vital not only for fertility but also for the maintenance of muscle mass, bone density, and mood stability. Low testosterone levels can result in symptoms such as fatigue, depression, and decreased libido. Hence, monitoring and maintaining hormonal balance is critical for men’s health and well-being. Additionally, lifestyle factors can influence testosterone levels, necessitating a holistic approach to male reproductive health.
In females, the ovaries perform multiple critical functions, particularly in producing estrogen and progesterone, which coordinate the menstrual cycle and influences reproductive functions. These hormones are pivotal in promoting the growth and maintenance of ovarian follicles during the follicular phase. Alongside FSH, estrogen encourages the maturation of the eggs and prepares the uterine lining for potential implantation. During ovulation, a surge in luteinizing hormone causes the release of a mature egg. Post-ovulation, progesterone levels rise, preparing the uterus for pregnancy, making it essential for maintaining early gestation. If fertilization does not occur, estrogen and progesterone levels drop, leading to menstruation. Furthermore, these hormones affect bone health and cardiovascular function, underscoring their importance beyond reproduction. Hormonal contraceptives manipulate this hormonal balance to prevent ovulation and regulate menstrual cycles, highlighting the versatility of ovarian hormones in reproductive health management. Disruptions in ovarian hormone levels can lead to conditions such as polycystic ovary syndrome (PCOS), affecting fertility and overall health. Understanding the regulation of these hormones aids in developing therapeutic approaches for managing reproductive issues.
Interplay Between Hormones in Reproductive Health
The intricate relationship between the hormones produced by the testes and ovaries significantly impacts overall reproductive health and systemic functions in both sexes. While testosterone is often considered a male hormone, it also plays roles in women’s health, influencing libido and bone density. Similarly, estrogen, while primarily a female hormone, is present in men where it regulates various functions, including sexual health and fat metabolism. The balance between these hormones is essential for maintaining optimal health, as imbalances can lead to conditions such as infertility, metabolic disorders, and increased risk of chronic diseases. There’s also emerging research on how environmental factors may affect endocrine functions, potentially leading to disruptions in hormone levels. These environmental endocrinological disruptors could impact both male and female reproductive capabilities and overall health. Awareness of these interactions highlights the need for a multifaceted approach to reproductive health that considers hormone balance, lifestyle choices, and environmental factors. Research into this field continues to elucidate the complexities of endocrine interactions, paving the way for innovative treatments and holistic approaches to reproductive health and wellness.
Along with hormones, the feedback mechanisms regulating the gonadal functions are complex and critical for homeostasis. For instance, the hypothalamus is key in the feedback loop of male hormone regulation. When testosterone levels rise, the hypothalamus decreases GnRH secretion, thereby lowering LH and FSH production from the pituitary. This feedback ensures testosterone is maintained within optimal levels to support various bodily functions. Conversely, a drop in testosterone leads to increased GnRH, enhancing LH and FSH production to stimulate testosterone synthesis. In females, the regulation is cyclical, correlating with the menstrual cycle. High levels of estrogen in the follicular phase provide negative feedback to the hypothalamus until ovulation occurs, then transitioning to a positive feedback prior to ovulation. This cycle underscores how hormonal fluctuations must be finely tuned to facilitate reproductive capabilities. Disruptions in any aspect of the feedback mechanism can lead to reproductive issues, underscoring the precision required for optimal endocrine health. Regular monitoring and understanding of how these processes work can assist in addressing reproductive disorders effectively.
Clinical Implications of Gonadal Hormones
The clinical implications of understanding the endocrine functions of the gonads are significant, particularly in addressing infertility and endocrine disorders. For men, low testosterone levels may be treated with hormone replacement therapy, which can enhance libido, energy levels and even mood stability. This treatment must be managed carefully due to potential side effects and the need for ongoing monitoring of hormone levels. In women, hormonal imbalances can lead to conditions like PCOS, endometriosis, or hormonal substitutions during menopause. Treatments often involve medications that balance estrogen and progesterone levels, allowing for better management of menstrual irregularities and systemic health. Moreover, in conditions like hypogonadism, understanding the role of these gonadal hormones can help tailor specific interventions that restore fertility or hormonal balance. The interplay of lifestyle factors, age, and environment presents additional considerations. As more research emerges on the connection between endocrine health and other systemic conditions, it becomes increasingly clear that a multidisciplinary approach is necessary for managing reproductive health effectively and improving overall quality of life.
Research into gonadal hormone functions reveals exciting implications for medicine and health. Advances in understanding hormonal roles can lead to the development of new treatments, enhancing the quality of life for hormone-related health conditions. For instance, the exploration of synthetic estrogens and androgens is paving the way for novel therapies that could address reproductive disorders more effectively. Moreover, the association between hormone levels and mood or cognitive functions demonstrates the need for integrated approaches to health. These developments highlight the importance of continued research into the roles of the testes and ovaries within the endocrine system. As knowledge expands, future therapies may involve gene editing, advanced hormonal regulation methods, and comprehensive lifestyle alterations tailored to individual hormonal profiles. In conclusion, the gonads’ endocrine functions are fundamental to reproductive health and broader physiological processes. Ongoing studies will undoubtedly yield further insights into the complexities of hormonal interplay, providing more robust strategies for tackling reproductive and endocrine health challenges.
The gonads are integral components of the endocrine system, influencing numerous aspects of human health. The coordination between the testes and ovaries exemplifies the intricate balance needed for optimal reproductive health. As research continues to unveil the complexities of hormonal interactions, healthcare professionals are better equipped to address the unique reproductive health needs of individuals. Understanding the roles of gonadal hormones is vital for developing personalized treatment options. This approach not only encompasses direct hormonal treatments but also considers lifestyle modifications and holistic health strategies. Continuous advancements in reproductive healthcare will allow for tailored approaches that enhance both fertility and general wellness. Therefore, ongoing research on the endocrine functions of the gonads remains crucial in uncovering new insights into hormone regulation and its applications in clinical practice. As we deepen our understanding, the future of endocrinology holds great promise for improving reproductive health outcomes, ultimately enriching the lives of countless individuals. The collaborative efforts of researchers, clinicians, and patients will drive the evolution of reproductive health practices geared towards individual needs, striving for a more balanced approach to end reproductive health.